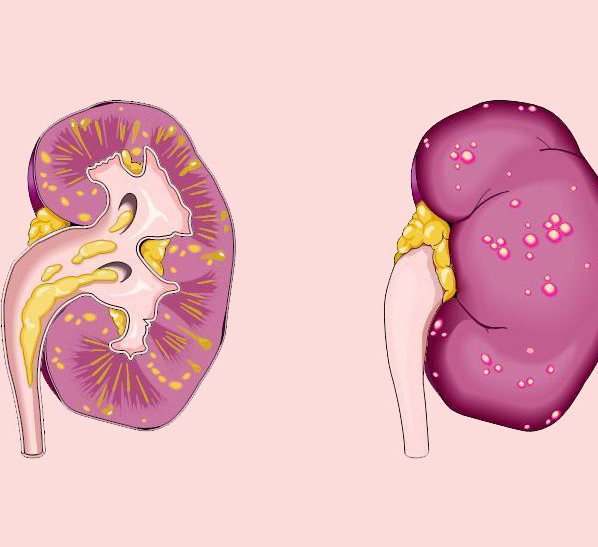
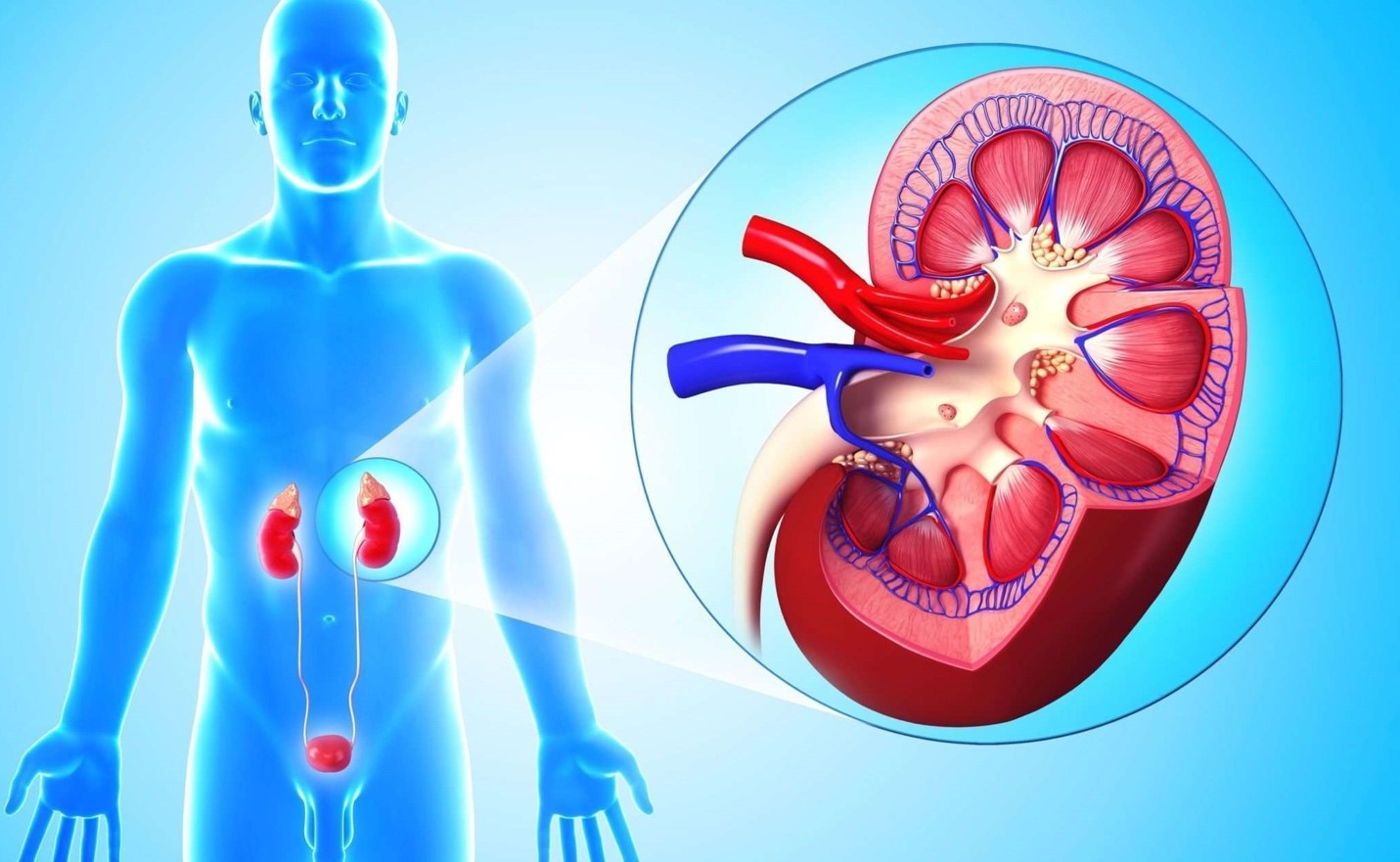
With age, central nervous system functions such as memory and intelligence (cognitive function) decline. This occurs both due to involutional processes in the brain and due to dysfunction of organs and systems (such as cardiovascular, excretory, digestive). In most older people, these changes do not go beyond the normal, generally accepted functioning. But about every tenth elderly person develops more severe disabilities, which leads to a loss of working capacity, social and domestic independence. This condition is defined as dementia (or dementia).
In modern society, thanks to the development of science, medical knowledge and the general progress of civilization, the life expectancy of a person has increased. So, according to some reports, the average life expectancy in Russia in the 19th century was 32 years, in the USSR in the 30s – 44 years, in the 60s – 69 years, in the 80s – 70 years. Currently, the average life expectancy is about 65 years, with women living longer than men by an average of 12 years. In connection with the increase in life expectancy, the prevalence, severity and social significance of persistent cognitive impairments leading to disability are increasing.
The development of dementia currently poses a difficult task for the patient’s relatives, his immediate environment and social services, as well as the health care system. The progression of cognitive impairment leads to the isolation of the patient from society and placement in specialized institutions (nursing homes, psychiatric clinics, psycho-neurological boarding schools, etc.). An increase in the number of patients with dementia leads to a decrease in the proportion of the working population, which is most relevant in our country, since there is a tendency to a decrease in life expectancy (in comparison with developed countries) and an increase in mortality among middle-aged people.
Among the main causes of dementia, it is not the aging of the brain that can be identified, but many diseases that cause continuous, single or multifocal damage to the cortex and subcortical structures of the brain. There are several main causes of dementia: primary dementia – associated with degenerative diseases (for example, Alzheimer’s disease), secondary dementia – associated with complications of diseases such as stroke, infections, alcoholism, trauma, cancer, cardiovascular diseases. Mixed forms of dementia are also distinguished.
Regardless of the causes of dementia, its manifestations consist in a global decrease in cognitive functions that disrupt social functioning (decreased attention, intelligence, memory, behavioral disorders in which episodes of aggression, anxiety, lack of self-care, etc. are possible).
In our country, the diagnosis of dementia is at a low level, often violations are detected quite late, because either relatives are trying to compensate patients for the lost social and everyday functions, or elderly people, living alone, are not of particular interest to others or become victims of criminal acts. Late diagnosis limits the ability of medicine to provide timely and sufficient care. You need to see a doctor at the first sign! There are modern drugs and algorithms for the treatment of patients with dementia, proven and validated in international studies.
As for individual families in which patients with dementia are identified, the situation sometimes reaches a dead end. So, for example, if an elderly person falls ill in a family, then the relatives have a difficult choice: to organize home care, or to shift it onto the shoulders of the state. In the first option, organizational difficulties are possible, since relatives mainly work and it is impossible to organize assistance to the patient 24 hours a day.
In the second variant, the manifestation of family feelings does not allow from the very first days to send an elderly person to a psychiatric hospital or a neuropsychiatric boarding school. If we talk about state aid for dementia, then today it is in its infancy: huge queues for neuropsychiatric hospitals, existing geriatric centers cannot cope with the large flow, and psychiatric hospitals are limited in funds for comprehensive care for such patients.
Dementia https://en.wikipedia.org/wiki/Dementia care is always based on the desire and interest of the patient’s relatives in creating the most comfortable conditions and the fastest help. Today, if certain conditions persist (absence of dangerous tendencies: pronounced aggression, suicidal behavior, decompensation of severe somatic pathology), competent and adequate outpatient care for patients with dementia is possible, including: diagnosis, selection of therapy, organization of qualified care, training of the patient’s relatives, monitoring of mental and somatic state.