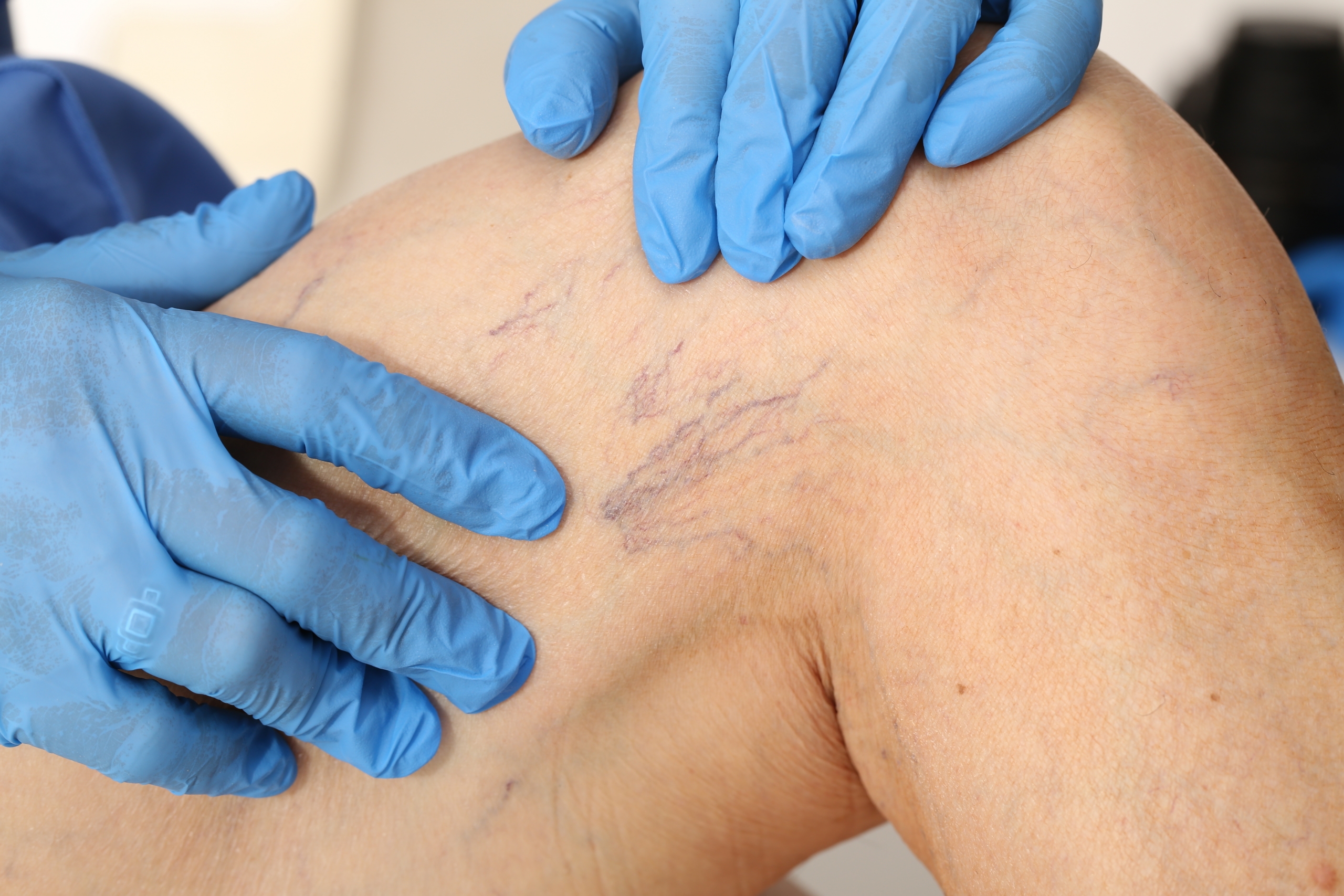
Varicose veins of the lower extremities, varicose veins (morbus varicosis) – persistent irreversible expansion and lengthening of the veins of the lower extremities as a result of an increase in pressure in them, which is caused by insufficiency of the venous valves due to a genetic defect, as well as aggravating factors (overweight, prolonged static loads, flat feet, hypertension, dyshormonal conditions, trauma, etc.). The name of the disease comes from the Latin word varix, varicis – bloating on the veins.
I will not dwell on the description of this disease, but I will consider only one of the modern methods of treatment and correction of varicose veins – microsclerotherapy. All over the world, vein sclerotherapy has been a leader in the treatment of varicose veins for decades.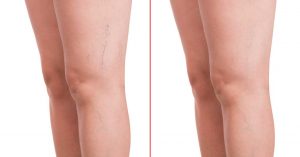
The low level of specialized care in Russia has led to the fact that among patients with varicose veins, patients with an advanced form of pathology still prevail, for whom nothing can help except surgery. Surgical treatment is indicated for 85-90% of primary patients with varicose veins. In St. Petersburg, the situation is more favorable, there are fewer patients with an advanced stage of the disease, so the percentage of those who can be helped without surgery, using less traumatic techniques, is higher.
Recently, interest in phlebosclerotherapy has increased for many reasons. This is also the general trend towards minimally invasive treatment. And a new economic approach to surgical diseases, when it becomes profitable to treat diseases in the early stages. And new diagnostic methods that reveal the features of the development of pathology, previously little or completely unknown. And, finally, this is a new generation of phlebosclerosing drugs that differ from the previous ones in safety, atrombogenicity and painlessness. Currently, the method is widely used in outpatient treatment practice, including in our center.
What veins can be hardened?
At the present stage, sclerotherapy can be applied to subcutaneous, intradermal, perforating veins of any localization. The effectiveness of the method decreases with a previously transferred thrombophlebitis and after previous unsuccessful sclerotherapy.
What are the indications for the procedure?
Sclerotherapy is indicated only for those patients who have objectively proven the absence of pathogenetic factors of varicose veins (the attending doctor will help to understand this):
no veno-venous discharges
segmental type of structure (isolated varicose veins of the tributaries of the main veins, expansion of intradermal veins (reticular varicose veins, telangiectasias = “snakes”, vascular “stars”)
permissible for the type of varicose veins without involving the main trunks in the process (deep veins are passable)
relapse of varicose veins that does not require reoperation
as an additional method for all forms of varicose veins before and after surgery
for obliterating veins outside the surgery area for cosmetic reasons.
What are the contraindications for the procedure?
skin infections in the injection area
diabetes mellitus (diabetic angiopathy)
immediate allergic reactions
severe bronchial asthma
atherosclerosis of the vessels of the lower extremities
pregnancy, lactation
deep vein thrombosis of the lower extremities, including relapses, inability to move
general serious condition
Indications and contraindications for manipulation are exposed only after the ultrasound method for examining the veins!
What is the method?
The goal of sclerotherapy is to inject an irritating chemical into the lumen of a vessel that causes irreversible damage to the endothelium with the development of fibrosis. If you connect the damaged walls of the vein with each other, then they grow together and the lumen of the vein is obliterated. Thus, treatment consists of two mandatory stages:
introduction of a phlebosclerosing substance into the lumen of the vessel
compression of the vein using special elastic bandages.
Since the process of creating a connective tissue scar at the site of the vascular lumen takes about a week, the compression (knitwear, elastic bandages) lasts at least seven days!
Due to the peculiarities of the anatomical connections between the superficial and deep venous arches, sclerotherapy on the veins of the foot is not performed.
Sclerotherapy is an outpatient method with a good cosmetic effect. It should be as painless as possible, easily portable, reliably performed and sufficiently traceless. The procedure is carried out under sterile conditions using disposable kits and takes from 30 minutes to 1 hour. We are successfully using one of the safest drugs – Ethoxysclerol. When using Ethoxysclerol, complications occur much less often, it does not cause local thrombosis and, moreover, is also an anesthetic (reduces pain). The optimal concentration of the drug depends on the diameter of the vein.
What are the complications of the procedure?
hyperpigmentation
edema
pain at the injection site
limited urticaria (a type of rash)
thrombophlebitis
fainting associated with fear of medical manipulation
relapse of the disease
If all the algorithms for performing this technique are observed, the occurrence of such complications is extremely rare.
Before starting treatment, you should have an idea of the essence of the procedure and its possibilities. It is impossible to achieve “ideal” legs in this case, but significant cosmetic correction is possible. The doctor should never promise the complete elimination of all vascular “asterisks”, “snakes”) – at best, in 3-6 sessions it will be possible to eliminate about 80-85%.
How to prepare for the procedure?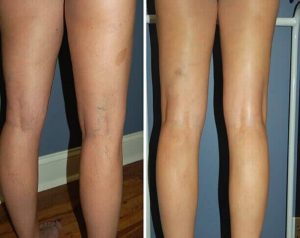
As a rule, no special training is required. General recommendations:
1 – 1.5 hours before the procedure, it is recommended to have a light snack;
before and on the eve of the procedure, do not use creams, lotions, epilation.
Immediately after sclerotherapy:
it is necessary to walk for 10-30 minutes (physical activity is not limited, walk for at least 1 hour every day);
you can not stand or sit for a long time;
avoid heat stress (baths, saunas, hot baths) for two months;
active physical activity is excluded for at least 3 days (gymnastics, aerobics, exercise bike).
Don’t worry if:
itching of the skin appeared at the injection site (usually observed within 1–2 hours, but in some cases it can periodically occur over several days);
there was a change in the color of the skin to a darker one along the affected vein (occurs in one of 20 patients, and can last for a year);
there was a small burn on the skin (it can form if a small amount of a sclerosing drug gets under the skin, it usually goes away on its own without additional treatment);
peeling of the skin began and a small wound appeared at the injection https://en.wikipedia.org/wiki/Injection_(medicine) site (occurs in one out of a hundred patients, and disappears without a trace within 1 to 2 weeks);
there is pain at the injection site and along the affected vein, can occur and worsen during physical exertion, and usually disappears after 3–9 days;
at the injection site, a red vascular mesh has formed, which lasts for several months and passes on its own.